Fremont Kaiser Patient Told He's Dying Via Tele-Robot Doctor Visit
SAN FRANCISCO (CBS/AP) -- Ernest Quintana's family knew he was dying of chronic lung disease when he was taken by ambulance to a hospital, unable to breathe.
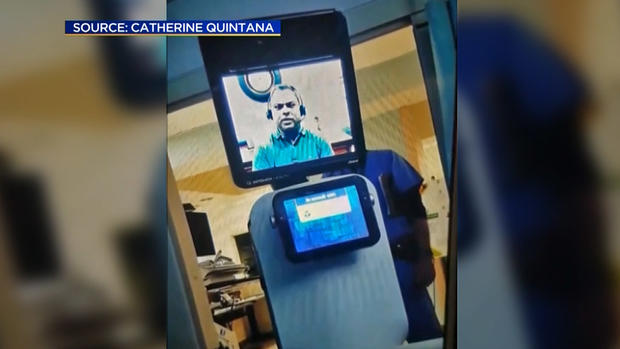
But they were devastated when a robot machine rolled into his room in the intensive care unit that night and a doctor told the 78-year-old patient by video call he would likely die within days.
"If you're coming to tell us normal news, that's fine, but if you're coming to tell us there's no lung left and we want to put you on a morphine drip until you die, it should be done by a human being and not a machine," his daughter Catherine Quintana said Friday.
Ernest Quintana died Tuesday, two days after being taken to the Kaiser Permanente Medical Center emergency department in Fremont.
Michelle Gaskill-Hames, senior vice president of Kaiser Permanente Greater Southern Alameda County, called the situation highly unusual and said officials "regret falling short" of the patient's expectations.
But the hospital also defended its use of telemedicine and said its policy is to have a nurse or doctor in the room at the time of remote consultations.
"The evening video tele-visit was a follow-up to earlier physician visits," Gaskill-Hames said in a written response. "It did not replace previous conversations with patient and family members and was not used in the delivery of the initial diagnosis."
Hospital officials say the technology doesn't replace in-person conversations with the patient and loved ones.
Granddaughter Annalisia Wilharm, 33, was alone with Quintana when a nurse popped in to say a doctor would be making his rounds. A robot rolled in and a doctor appeared on the video screen.
Wilharm figured the visit was routine. She was astonished by what the doctor started saying.
"This guy cannot breathe, and he's got this robot trying to talk to him," she said. "Meanwhile, this guy is telling him, 'So we've got your results back, and there's no lung left. There's no lung to work with.'"
Wilharm said she had to repeat what the doctor said to her grandfather, because he was hard of hearing in his right ear and the machine couldn't get to the other side of the bed.
"So he's saying that maybe your next step is going to hospice at home," Wilharm is heard saying in a video she recorded of the visit. "Right?"
"You know, I don't know if he's going to get home," the doctor says.
Steve Pantilat, chief of the palliative medicine division at University of California, San Francisco, said he doesn't know the details in the case but that the robot technology has done wonders for patients and their families, some of whom are too far away for in-person visits.
The video meetings are warm and intimate, he said, adding that not all in-person discussions have empathy and compassion.
"No matter how well we deliver very difficult news, it's sad and it's hard to hear," he said.
Wilharm said her grandfather, a family man who kept every childhood drawing he ever gave her, deserved better. She said that after the visit, he gave her instructions on who should get what and made her promise to look after her grandmother.
"He was such a sweet guy," she said.
KPIX received the following statement Friday night from Kaiser Permanente Northern California:
"On behalf of Kaiser Permanente and our caregivers in Fremont, we offer our sincere condolences. It is always deeply painful to lose a beloved family member and friend. We take this very seriously and have reached out to the family to discuss their concerns.
In every aspect of our care, and especially when communicating difficult information, we do so with compassion in a personal manner. The use of the term "robot" is inaccurate and inappropriate. This secure video technology is a live conversation with a physician using tele-video technology, and always with a nurse or other physician in the room to explain the purpose and function of the technology. The technology allows a small hospital to have additional specialists such as a Board-certified critical care physician available 24/7, enhancing the care provided and bringing additional consultative expertise to the bedside.
Our physicians and nurses were in regular, in-person communication with the patient and family about his condition from the moment he entered our hospital. The evening video tele-visit was a follow-up to earlier physician visits – it did not replace previous conversations with patient and family members and was not used in the delivery of the initial diagnosis.
This is a highly unusual circumstance. Kaiser Permanente, like every health care provider, is continuously learning how best to integrate technology into patient interactions. Patients are accustomed to physicians following up by phone. With new technology, we can extend that to offer video interactions over smart phones or video screens in the hospital. That said, we don't support or encourage the use of technology to replace the personal interactions between our patients and their care teams – we understand how important this is for all concerned, and regret that we fell short of the family's expectations. We will use this as an opportunity to review how to improve patient experience with tele-video capabilities."
© Copyright 2019 CBS Broadcasting Inc. All Rights Reserved. The Associated Press contributed to this report